Category: News
Visiting Medical Student’s last day
Left – Right: Maryam Ali Khan, Chin Siang Ong, Jason Juncheng Huang (visiting medical student from Singapore), Narutoshi Hibino, Takuma Fukunishi, Huaitao Zhang in the Division of Cardiac Surgery office (Zayed 7107)
“Last words”: It was a great privilege for me to be part of Dr Hibino’s research team during my 1 month elective at Johns Hopkins University. The research that Dr Hibino and his team pursues inspires me greatly, as I’ve witnessed the dedication that the team puts in to the work that they believe so much in. Being able to participate in the weekly research meetings has enlightened me to the practice of cutting-edge translational research, an opportunity I am very thankful for. It was a great learning experience interacting with the team and assisting in some of the research work.

New Publication: Preclinical study of patient-specific cell-free nanofiber tissue-engineered vascular grafts using 3-dimensional printing in a sheep model.
J Thorac Cardiovasc Surg. 2017 Apr;153(4):924-932. doi: 10.1016/j.jtcvs.2016.10.066. Epub 2016 Nov 14.
Preclinical study of patient-specific cell-free nanofiber tissue-engineered vascular grafts using 3-dimensional printing in a sheep model.
Fukunishi T1, Best CA2, Sugiura T2, Opfermann J3, Ong CS1, Shinoka T2, Breuer CK2, Krieger A3, Johnson J4, Hibino N5.
Author information
- 1. Department of Cardiac Surgery, Johns Hopkins Hospital, Baltimore, Md.
- 2. Tissue Engineering and Surgical Research, Nationwide Children’s Hospital, Columbus, Ohio.
- 3. The Sheikh Zayed Institute for Pediatric Surgical Innovation, Children’s National Medical Center, Washington, DC.
- 4. Nanofiber Solutions Inc, Columbus, Ohio.
- 5. Department of Cardiac Surgery, Johns Hopkins Hospital, Baltimore, Md. Electronic address: nhibino1@jhmi.edu.
Abstract
BACKGROUND:
Tissue-engineered vascular grafts (TEVGs) offer potential to overcome limitations of current approaches for reconstruction in congenital heart disease by providing biodegradable scaffolds on which autologous cells proliferate and provide physiologic functionality. However, current TEVGs do not address the diverse anatomic requirements of individual patients. This study explores the feasibility of creating patient-specific TEVGs by combining 3-dimensional (3D) printing and electrospinning technology.
METHODS:
An electrospinning mandrel was 3D-printed after computer-aided design based on preoperative imaging of the ovine thoracic inferior vena cava (IVC). TEVG scaffolds were then electrospun around the 3D-printed mandrel. Six patient-specific TEVGs were implanted as cell-free IVC interposition conduits in a sheep model and explanted after 6 months for histologic, biochemical, and biomechanical evaluation.
RESULTS:
All sheep survived without complications, and all grafts were patent without aneurysm formation or ectopic calcification. Serial angiography revealed significant decreases in TEVG pressure gradients between 3 and 6 months as the grafts remodeled. At explant, the nanofiber scaffold was nearly completely resorbed and the TEVG showed similar mechanical properties to that of native IVC. Histological analysis demonstrated an organized smooth muscle cell layer, extracellular matrix deposition, and endothelialization. No significant difference in elastin and collagen content between the TEVG and native IVC was identified. There was a significant positive correlation between wall thickness and CD68+macrophage infiltration into the TEVG.
CONCLUSIONS:
Creation of patient-specific nanofiber TEVGs by combining electrospinning and 3D printing is a feasible technology as future clinical option. Further preclinical studies involving more complex anatomical shapes are warranted.
Copyright © 2016. Published by Elsevier Inc.
KEYWORDS:
3D printing; Fontan circulation; cell-free tissue engineering; congenital heart disease; electrospun nanofibers; patient-specific; preclinical study; sheep model; tissue-engineered vascular graft
New Publication: Left heart decompression in patients supported with extracorporeal membrane oxygenation for cardiac disease.
Postepy Kardiol Interwencyjnej. 2017;13(1):1-2. doi: 10.5114/aic.2017.66179. Epub 2017 Mar 10.
Left heart decompression in patients supported with extracorporeal membrane oxygenation for cardiac disease.
Author information
- 1. Division of Cardiac Surgery, Johns Hopkins Hospital, Baltimore, MD, USA.
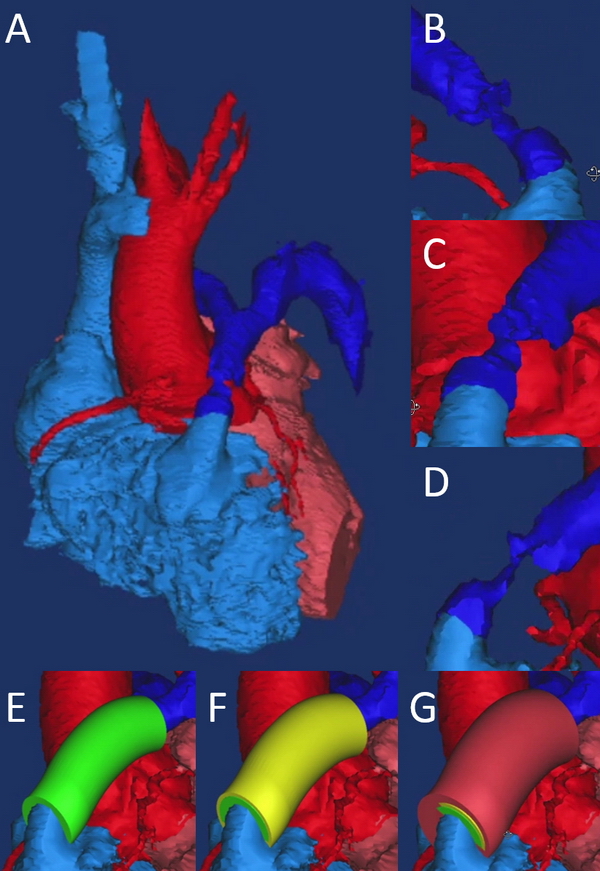
Accepted Publication: Virtual Surgery for Conduit Reconstruction of the Right Ventricular Outflow Tract
Virtual Surgery for Conduit Reconstruction of the Right Ventricular Outflow Tract
Chin Siang Ong1, Yue-Hin Loke2, Justin Opfermann2, Laura Olivieri2, Luca Vricella1, Axel Krieger3, Narutoshi Hibino1.
1. Division of Cardiac Surgery, Johns Hopkins Hospital, Baltimore, MD, USA
2. Division of Cardiology, Children’s National Health System, Washington DC, USA
3. Sheikh Zayed Institute for Pediatric Surgical Innovation, Children’s National Health System, Washington DC, USA
Journal: World Journal for Pediatric and Congenital Heart Surgery